Disclaimer: I am not a brain scientist, psychiatrist, nor a psychologist. I’m just someone who likes to read and write a lot and has lifelong personal experience with the topics covered by this article. If you want to learn more about these subjects, I recommend that you do your own research. Ask your doctor for medical advice, but keep in mind that the world-class scientists that wrote the peer-reviewed studies you will find on Google might be a more reliable source of information.
I think it’s a mistake to overemphasise the importance of diagnostic labels in mental health. In my experience, the boundaries between different mental disorders are very blurry. Asperger syndrome can turn into executive dysfunction (ADHD) can turn into depression can turn into anxiety can turn into mania can turn into psychosis (schizophrenia). Personality disorders are usually due to childhood trauma and can also trigger these conditions.

The most correct thing any mental health expert can say about any individual with a mental disorder is that they are mentally ill, and beyond that, it’s just attaching labels to things. What you actually need to do if you struggle with mental illness is try to untangle the mess: Are there fundamental causes? Common themes? Are there vicious cycles to break?
Further, there are no universal surefire treatments for any mental illness. Putting labels on different aspects of this black ball of string that is called mental illness is useful in that it can help you identify the knots in it, but there is no straight path from a diagnostic label to a medication that is guaranteed to work. Some of the knots might be mistaken beliefs or destructive reaction patterns that could be adjusted.
My belief is that there are usually one or more neurological issues involved, but there may be fewer of them than you might imagine. It’s just that you have a handful of them that have ballooned and branched out, that were then compounded when they sent you spiralling into self-destructive patterns of thinking.
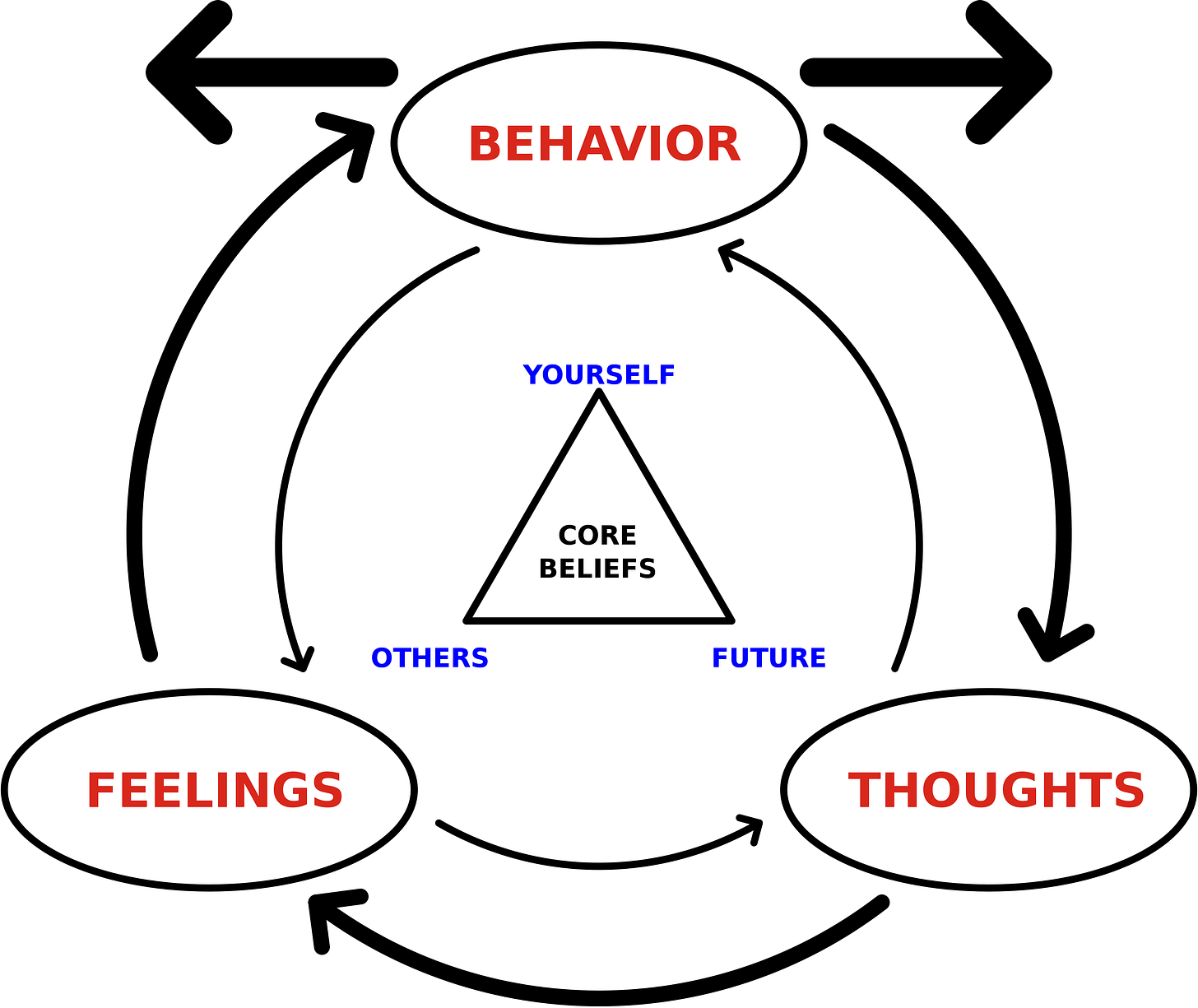
Lately, I’ve been playing with reinventing the thoughts-feelings-behaviour diagram used when teaching cognitive-behavioural therapy — a form of treatment in which an intervention is carried out by a therapist at one of three problem sites: behaviour, thinking, or feelings.
The Wikipedia article illustrates it as a three-way cycle, like this:
This implies that the processes of thinking, acting and feeling happen in a serial cycle, but this isn’t true. These functions of the brain occur in parallel, not in series. A flowchart doesn’t properly describe that.
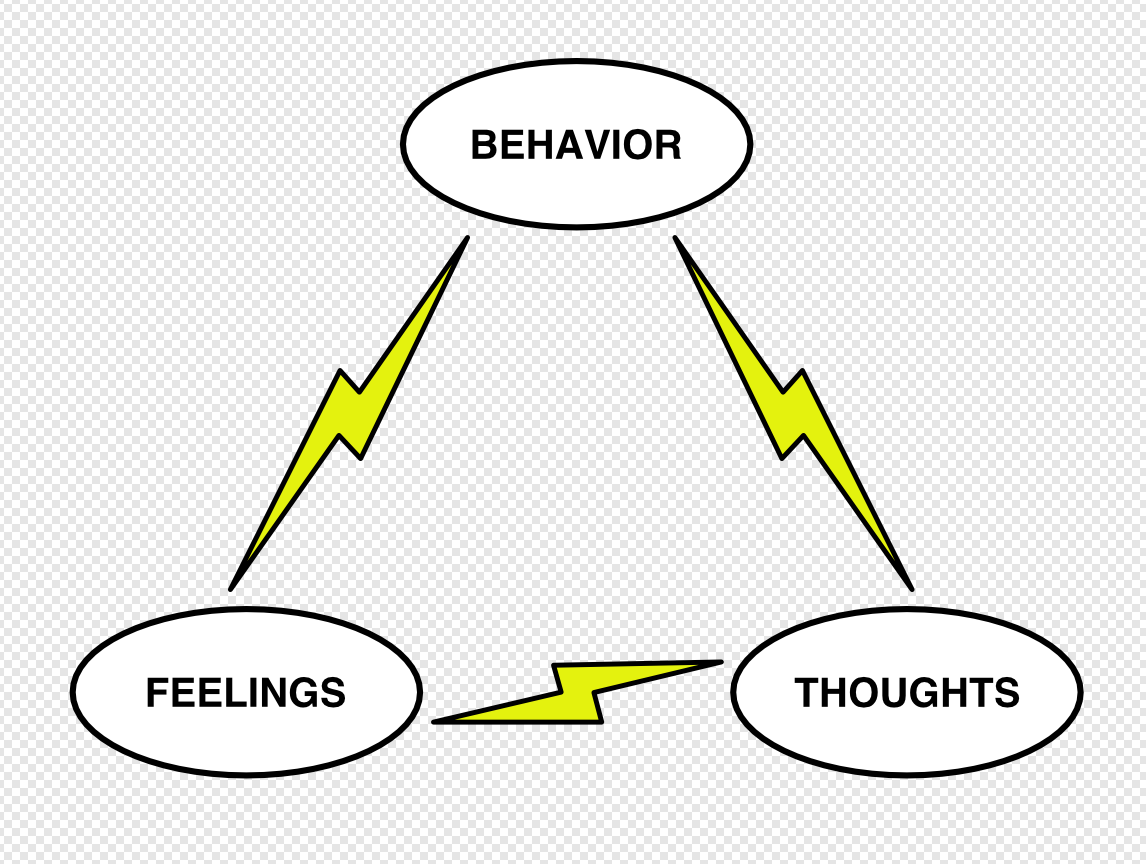
Here’s a basic attempt at a chart that gets the idea across better:
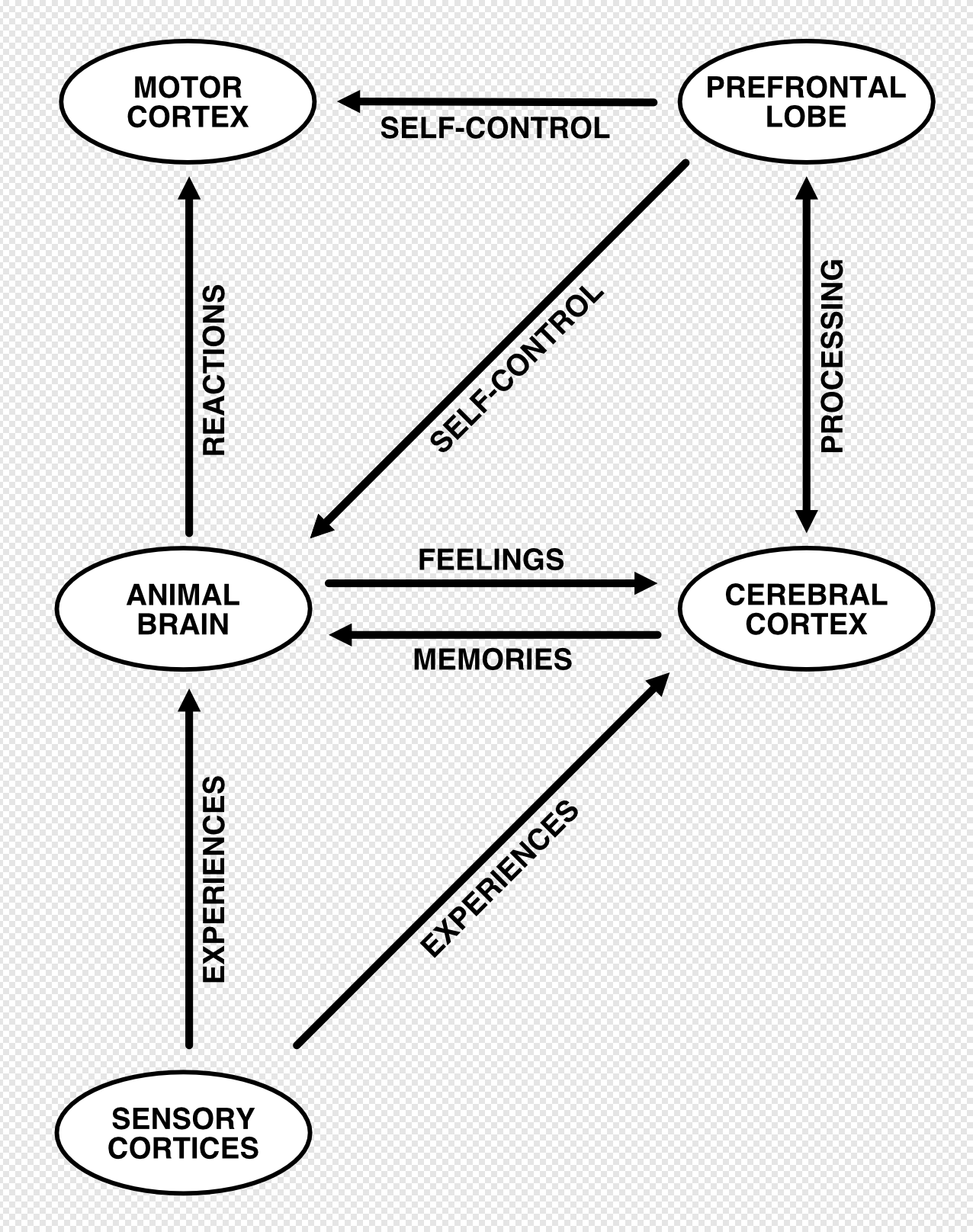
They are influencing each other all the time, in real-time, like lightning bolts between clouds. In order to refine this idea to reflect modern neuroscience, more moving parts and some relabelling is needed:
Now, this chart isn’t accurate. No chart of the brain can be, but the general idea is this: In lower animals, the animal brain — also known as the monkey or lizard brain — is more or less all there is. It gets a stimulus, it responds and that’s it. In higher animals, the cerebral cortex is there to do more analysis to interpret things — it thinks, and it hands this information to the prefrontal cortex, which makes a decision and sends activating and suppressing commands back to the animal brain — for example to encourage or inhibit emotions — or to the motor cortices — to encourage or inhibit actions.
The prefrontal cortex is the command centre of the human brain. When inactive, the animal brain basically just carries on doing what it would have done in an animal. When it’s active however, higher cognitive processes can influence behaviour. The cerebral cortex and the prefrontal cortex are on the phone with each other constantly, forming a feedback loop.
In people with ADHD — a disorder of attention, focus, motivation, organisation, planning and emotional regulation — there’s plenty of activity in the cerebral cortex, but the prefrontal cortex is having some issues. If you inject some extra dopamine into the prefrontal cortex using stimulants, it gets its powers back, a bit like if you feed spinach to Popeye.
You might say that the primary trait of ADHD is a lack of active control of natural animalistic behaviours. There is no lack of awareness as such, since there’s no problem with the cerebral cortex. It’s just that translating thought into appropriate action or inaction is difficult. The prefrontal cortex can’t get itself together because it’s starved of dopamine — dopamine being the neurotransmitter that convinces the prefrontal cortex that perhaps it should take a more active approach and step in to organise things before they get out of hand. Without the dopamine, it can only watch on as the animal brain acts like a fool.
ADHD is relevant to anyone with a mental illness because it has as comorbidities (ensuing disorders) most of the common mood disorders, such as bipolar disorder, anxiety, depression, and so on. The issue is that a malfunctioning prefrontal cortex can lead to an emotional instability issue. Instead of keeping it together, you lose yourself in the moment and get carried away.
I feel this lies at the heart of many mental disorders. The problem is — when you boil it down to its essentials — that you can’t control your feelings, and that’s exactly what the prefrontal cortex is responsible for. Making sure that your prefrontal cortex is functioning properly is crucial for… everything.
When you receive any diagnosis from a psychiatrist, keep this in mind. These issues could be corroborating to make things worse for you. You have to work like a detective to untangle the mystery, spot the perpetrators and catch them red-handed. This is how you work to improve your well-being. It will reduce your dependence on a therapist if you learn to self-monitor and self-modify like this.